Inflammasome activation at the crux of severe COVID-19
- David Ojcius
- Aug 12, 2021
- 2 min read
Review of evidence that #SARSCoV2#coronavirus directly or indirectly activates #inflammasomes, leading to secretion of IL-1 family cytokines (IL-1beta and IL-18), and pyroptosis, an inflammatory form of cell death.
The #COVID19 pandemic, caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), results in life-threatening disease in a minority of patients, especially elderly people and those with co-morbidities such as #obesity and #diabetes. Severe disease is characterized by dysregulated cytokine release, pneumonia and acute lung injury, which can rapidly progress to acute respiratory distress syndrome, disseminated intravascular coagulation, multisystem failure and death. However, a mechanistic understanding of COVID-19 progression remains unclear. Here we review evidence that SARS-CoV-2 directly or indirectly activates inflammasomes, which are large multiprotein assemblies that are broadly responsive to pathogen-associated and stress-associated cellular insults, leading to secretion of the pleiotropic IL-1 family cytokines (IL-1β and IL-18), and pyroptosis, an inflammatory form of cell death. We further discuss potential mechanisms of inflammasome activation and clinical efforts currently under way to suppress inflammation to prevent or ameliorate severe COVID-19.
Read more at:

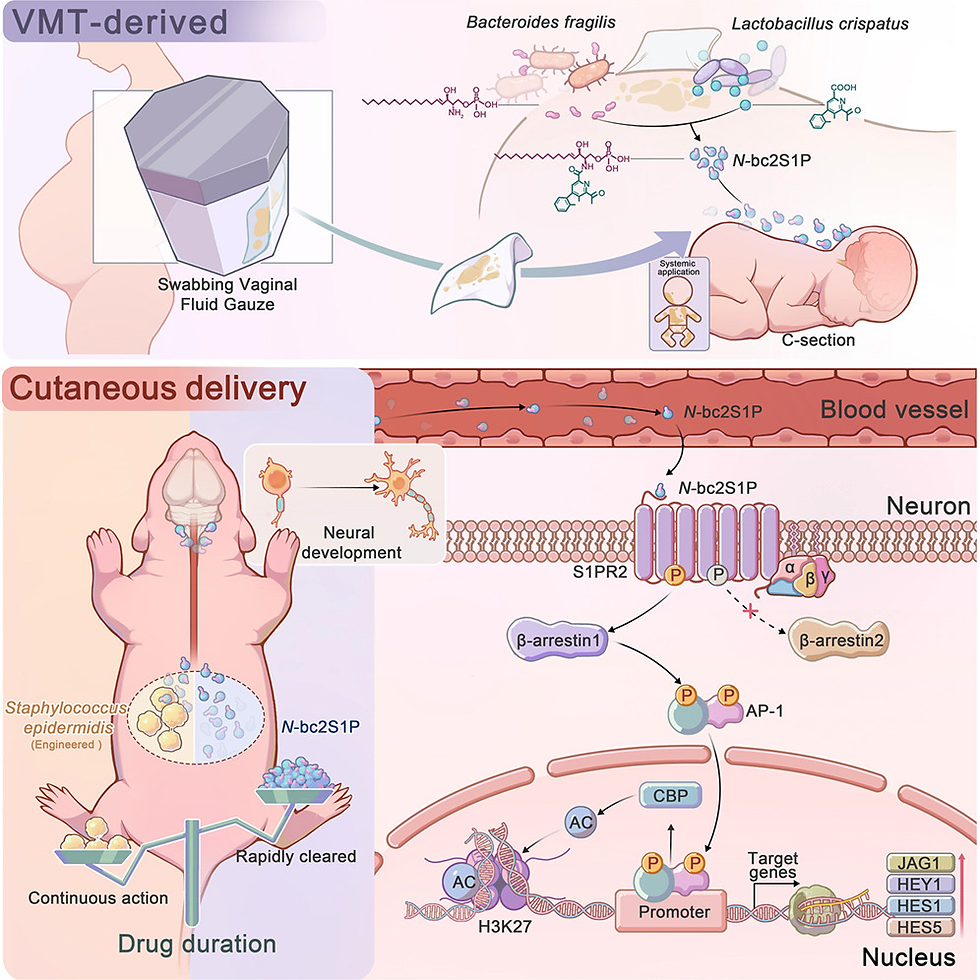
Figure: Virus intrinsic mechanisms (red arrows): severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) virions enter epithelial cells via angiotensin-converting enzyme 2 (ACE2) and can enter monocytes by binding to anti-spike antibodies followed by Fc receptor for IgG (FcγR)-mediated internalization. Upon translation of the viral genome, the viroporins ORF3a and E can trigger K+ efflux or Ca2+ influx to promote NLRP3 activation. Viral N protein can bind directly to NLRP3, resulting in its activation. Host-intrinsic mechanisms (blue arrows): oxidation of lung surfactant phospholipids results in oxidized phospholipids (oxPLs), which can activate caspase 4 and/or caspase 5 to promote noncanonical inflammasome activation. Complement products such as C5a can activate NLRP3 by promoting accumulation of reactive oxygen species (ROS). ATP released by dead cells binds to P2X7 receptor, which causes K+ efflux and NLRP3 activation. Dead cells, bacterial co-infection or damaged mitochondria can result in cytosolic double-stranded DNA (dsDNA), which activates the AIM2 inflammasome. NLRP3 and AIM2 inflammasome assembly activates caspase 1, which cleaves full-length (FL) gasdermin D (GSDMD) into amino-terminal (NT) and carboxy-terminal (CT) fragments. The GSDMD NT fragment binds to the plasma membrane, oligomerizes and inserts itself as a pore. Caspase 1 also cleaves pro-IL-1β and pro-IL-18 into their mature forms, which are released through the GSDMD pore. IL-1β can activate macrophages to secrete additional proinflammatory cytokines such as IL-6. Pyroptosis results after further membrane damage, which releases lactate dehydrogenase (LDH) and is associated with the formation of tissue factor-enriched extracellular vesicles (EVs). CRP, C-reactive protein; ERGIC, endoplasmic reticulum–Golgi intermediate compartment; TNF, tumour necrosis factor.


Comments